As a complex condition that varies widely from patient to patient, there are four main factors that go into how a patient’s scoliosis is classified: age, size of curve, location of curve, and the cause of the condition.
Scoliosis Classification
edical conditions are classified for multiple reasons. Common classifications such as a patient’s age, condition-type, and condition severity help nurses, doctors, and surgeons know what they’re dealing with when they are treating a patient.
When it comes to scoliosis specifically, having a more thorough understanding of a patient’s scoliosis from a number of angles increases the likelihood of successfully treating the condition.
Knowing the type and location of a patient’s curvature can also help predict what symptoms they are likely to experience, and this has a great impact on how the patient experiences and lives with the condition.
When it comes to classifying scoliosis, age, size of curve, location of curve, and the condition’s cause helps give medical professionals a more comprehensive understanding of a complex 3-D condition.
Patient’s Age
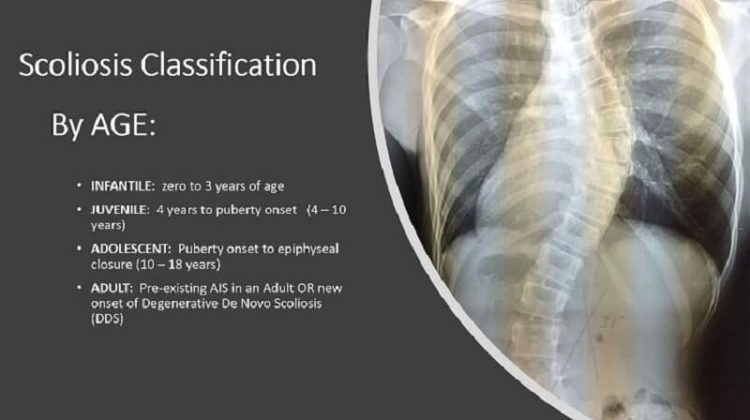

The age of a patient with scoliosis is the first point of classification. When it comes to scoliosis, this is particularly important.
The patient’s age will determine how much progression is likely to occur. As scoliosis is a progressive condition with no known cause (in most cases) or cure, treatment focuses on how to slow down or stop the progression of the curvature.
Scoliosis can affect infants, juveniles, adolescents, and adults.
Infantile Scoliosis
The age group that makes up the category of ‘infantile scoliosis’ is from birth to the age of 3. Most cases of infantile scoliosis fall into one of two categories: idiopathic or congenital.
Idiopathic means there is no known cause for the condition and experts don’t know why the curvatures form.
Cases of congenital scoliosis are different from infantile idiopathic scoliosis because there is a known cause. When a baby is born with a bone malformation, the deformity develops before birth and can lead to the development of a crooked spine.
In a healthy spine, the vertebrae are stacked on top of each other like bricks. In cases of congenital scoliosis, one of those bricks is shaped like a triangle, rather than a rectangle like the other vertebrae. That malformed triangular vertebrae causes the spinal cord to tilt or bend and develop a curvature.
The category of infantile scoliosis only accounts for 1 percent of idiopathic scoliosis cases in children, and approximately 60 percent of infantile scoliosis patients are male.
Juvenile Scoliosis
The age group that makes up the category of ‘juvenile scoliosis’ is from 4 to 10 years of age. For children of this age, I consider treatment to be especially important.
This category can be made up of cases of infantile scoliosis who were undiagnosed and moved into the ‘juvenile’ category with their condition, or it can be cases of idiopathic juvenile scoliosis where the curvature develops for unknown reasons.
For parents going with the traditional treatment route, they will likely be told that waiting to see how the condition progresses at this stage is a good idea. This approach is something I disagree with, especially at this age.
Juveniles have the highest likelihood of curvature progression because they have not yet gone through the big growth spurts associated with puberty. As growth is the main known cause of progression, I like to be proactive with juveniles and initiate treatment right away to minimize the risks of progression as they age and grow.
Catching a curve before it progresses, achieving a reduction, and holding that reduction through puberty is the best way to manage the condition’s progression.
The category of juvenile idiopathic scoliosis makes up approximately 10-to-15 percent of idiopathic scoliosis cases in children, and statistically speaking, girls are more likely to develop juvenile scoliosis than boys.
Adolescent Scoliosis
The age group that makes up the category of ‘adolescent scoliosis’ is from 10 to 18, and this age group represents the most common age of diagnosis and the most common type of scoliosis. At this stage, growth and progression is the main concern as puberty can exacerbate the condition’s progression and related symptoms.
The vast majority of adolescent scoliosis cases are idiopathic. While we can diagnose the condition and treat it through monitoring and achieving a reduction, we simply don’t know what variables combine to cause the initial development of the spinal curvature.
Although the cause of adolescent idiopathic scoliosis is unknown, theories involving genetic predispositions, environmental factors, hormone imbalance, muscle imbalance, and asymmetric growth are constantly being explored. What I always tell my patients and their caregivers is that knowing the cause would be comforting, but it wouldn’t necessarily change the chosen treatment path or affect its efficacy.
Adolescent idiopathic scoliosis is found in approximately 4 out of 100 adolescents.
Adult De Novo Scoliosis
The age group that makes up the ‘adult do novo scoliosis’ category is 18+. At this stage, pain management is often a large part of treatment as adults experience scoliosis-related pain very differently from adolescents.
‘De novo’ refers to cases of adults who develop the condition with no prior history of scoliosis, meaning they didn’t carry the condition with them, undiagnosed, from adolescence and into adulthood.
While there are cases of adult idiopathic scoliosis, most cases of adult de novo scoliosis have one of the three known causes:
- degenerative, traumatic, or pathological.
Size of Curve
Once a condition is classed by age, the next step is to document the size of the patient’s curve. This is done via X-ray and what’s known as a Cobb angle measurement.
The Cobb angle measures the degree to which the spine curves and rotates away from a straight alignment, and the apex of the curve helps determine the measurement. The apex refers to the vertebra or disk with the largest rotation or farthest deviation from the vertebral column’s center. End vertebrae have the largest tilt towards the curve’s apex, and these are used to measure the Cobb angle.

The higher the Cobb angle measurement, the more severe the condition is. The measurement will class the condition as mild, moderate, or severe.
- Mild scoliosis – conditions where the Cobb angle measures at 25 degrees or less.
- Moderate scoliosis – conditions where the Cobb angle measures between 25 and 40 degrees.
- Severe scoliosis – conditions where the Cobb angle measures at 40+ degrees for adolescents and 50+ degrees for adults.
Once the Cobb angle measurement is taken and the patient’s condition is placed on the mild-to-severe scale, an appropriate treatment plan can be devised and implemented.
Location of Curve
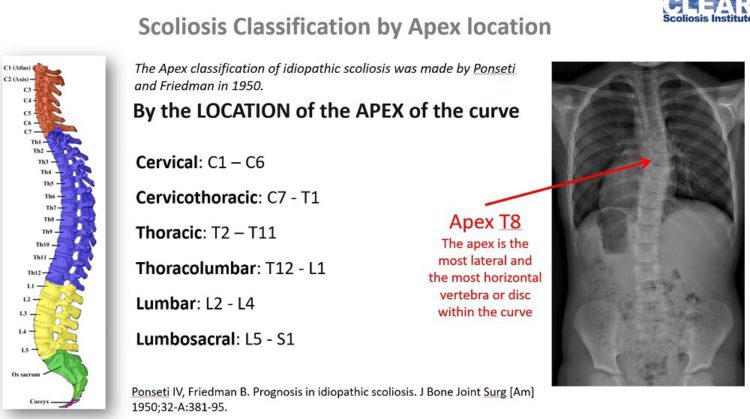
While there are numerous systems in place for classifying types of scoliosis curves, the most common and reliable categorizes curves based on their location within the spine and in which direction they bend.
Terms such as ‘thoracic’, ‘lumbar’, and ‘thoracolumbar’ refers to where the curve is located along the spine, and terms like ‘dextroscoliosis’ and ‘levoscoliosis’ refer to the direction of the curve: left or right.
Thoracic Scoliosis
- Thoracic scoliosis refers to a curvature in the middle portion of the spine
- Curves located in the thoracic part of the spine are the most common
- Thoracic scoliosis often causes a deformity of the rib cage, in addition to the spine
- The asymmetrical rib cage can cause asymmetrical shoulders where one appears higher than the other
- Legs can also appear to be different lengths
Lumbar Scoliosis
- Lumbar scoliosis refers to a curvature located in the lower part of the spine
- Lumbar scoliosis often causes one hip to sit higher than the other
- Legs appearing to be different lengths is also common
- Lumbar scoliosis can be degenerative in adults who are over the age of 50
Thoracolumbar Scoliosis
- Thoracolumbar scoliosis refers to cases where the curve is comprised of both lower-thoracic and upper-lumbar vertebrae
- Most cases of congenital scoliosis are thoracolumbar occurring before birth between the third and sixth week of gestation
- Can be a secondary effect of neuromuscular conditions such as cerebral palsy or spina bifida
- In thoracolumbar scoliosis, curves often bend towards the right
- More females than males will develop thoracolumbar scoliosis
Dextroscoliosis
- Dextroscoliosis is characterized by a sideways curvature that bends to the right
- Dextroscoliosis is one of the most common scoliosis curvatures
- Gives the spine an ‘S’ or ‘C’ shape, depending on the condition’s severity
- Most commonly affects the thoracic spine area
- Most associated with children between 10 and 15 years of age going through their first big growth spurt
- Can be caused by a variety of connective tissue or muscle disorders common in older individuals
Levoscoliosis
- Levoscoliosis is characterized by a sideways curvature that bends to the left
- Most often, it affects the lumbar spine, but it can also affect the thoracic spine
- When the thoracic spine is involved, it can put pressure on the organs and lead to impairments of the heart and lungs
- Mild cases of levoscoliosis can be asymptomatic and might not even progress
- Severe cases of levoscoliosis can cause asymmetries of the shoulders and hips and lung impairment
- Most often, levoscoliosis is not a particularly painful condition
- Levoscoliosis has no known cause
- It is commonly present at birth in the form of congenital scoliosis
- Levoscoliosis can also be a secondary development of muscle and tissue disorders such as muscular dystrophy
Cause of the Condition
While I point out to patients all the time that knowing the cause of scoliosis is not necessary to develop an effective treatment plan, in terms of classifying the condition, it is an important aspect.
While 80 percent of known diagnosed scoliosis cases are idiopathic, the remaining 20 percent have known causes that can help direct the course of treatment and prepare the patients for what symptoms they can expect to experience.
Following is a list of condition-cause types that further classify the condition:
- Idiopathic Scoliosis – when the condition has no known single cause
- Degenerative Scoliosis – cases where a spinal curvature develops due to degenerative changes to the spine that occur as a natural part of the aging process. This is most common in older individuals.
- Traumatic Scoliosis – cases where a spinal curvature is caused due to a trauma to the spine, such as a fall or car accident.
- Neuromuscular Scoliosis – cases where children develop scoliosis as a result of having medical conditions that impair the body’s ability to control the muscles supporting the spine. Most often caused by muscular dystrophy, cerebral palsy, and spina bifida.
- Pathological Scoliosis – cases where tumors are present. When a tumor is pressed against the spine, it can push the spine and cause a curvature to develop.
- Congenital Scoliosis – cases where there is a bone malformation that took place during gestation. The failure of the bones to form properly leads to an abnormal spinal curvature.
- Adult De Novo Scoliosis – cases where scoliosis develops in adults when there is no past history of the condition. While some cases of idiopathic scoliosis can develop in adults, most often the condition is classed as degenerative, traumatic, neuromuscular, or pathological.
Conclusion
When a patient first receives a scoliosis diagnosis, it’s a scary time. Patients and their caregivers don’t know what to expect. They don’t know what life is going to look like in the near and distant future.
Patients and caregivers who are proactive want to know as much about the condition as possible so they can choose the best course of treatment. Classifying a patient’s medical condition is not just for the medical professionals, it’s also for the patient’s benefit. Knowing where a condition places on its classification scale helps determine the best course of treatment, as well as what symptoms a patient is likely to experience.
Scoliosis is a complex condition that can take different forms; understanding these different forms is crucial when it comes time to initiate a treatment plan that offers the patient the best chance of symptom relief and curvature reduction.
When a patient’s condition is classified, the answer to each aforementioned category becomes that patient’s condition type. For example, if a patient is 14 years old with a 27-degree spinal curvature in the middle part of the back that bends to the right with no known cause, the condition would be classified as ‘adolescent idiopathic moderate thoracic dextroscoliosis’.
Here at the Scoliosis Reduction Center®, every patient receives a customized treatment plan based on the nature of their condition and any related symptoms they are experiencing. Regardless of when you received your initial diagnosis or what type of scoliosis you have, it’s never too late to start treatment and move towards managing the condition proactively, rather than passively observing the condition and letting it manage you.






