Severe Scoliosis
Further Progression is Certain!
While more commonly diagnosed in adolescence, scoliosis can develop at any age. As a highly-complex condition, it can take many forms and range from mild to moderate, and severe. Keep reading to find out how we classify a patient’s condition on its severity scale and determine what makes scoliosis ‘severe’.
When scoliosis is first diagnosed, it’s classified on the condition’s severity scale; this is done via a measurement obtained during X-ray known as the ‘Cobb angle’. If a patient’s Cobb angle measures at 40+ degrees and includes rotation, it’s classified as ‘severe scoliosis’.
There are so many factors that play into a person’s experience with scoliosis. From diagnosis to symptoms, potential complications and treatment, no two patients will have the same experience. This is due to a large number of variables, one of which is the condition’s severity level. Before we look at ‘severe scoliosis’ specifically, let’s first take a look at how a condition is diagnosed and classified.
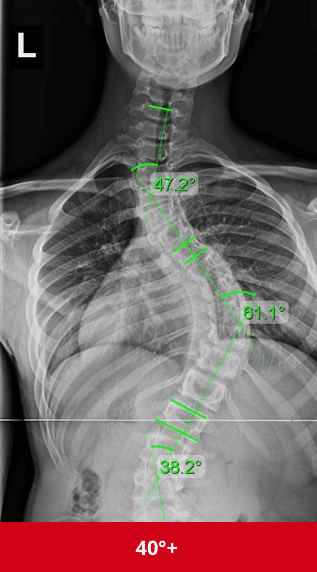
Diagnosing Scoliosis
As we are specifically talking about severe scoliosis, I first want to be clear that when I see a patient with severe scoliosis, these are extreme cases. While seeing a 100+ degree curvature is familiar to me, it’s never a simple treatment approach.
An extreme case is an extreme case, regardless of how many times I have treated similar forms of the condition.
Also, the patients who come to me, already in the severe stage of progression, have consulted with a spinal surgeon and refused to undergo the spinal-fusion surgery recommended to them.
When these patients come to me, we work proactively to move forward in their treatment with our alternative functional treatment approach.
When it comes to diagnosing scoliosis, the majority of my patients are adolescents; this is because the condition’s most common form is adolescent idiopathic scoliosis (AIS), and these cases account for 80 percent of known diagnosed cases.
The remaining 20 percent have known causes, such as congenital, neuromuscular, degenerative, and traumatic.
When a patient is first diagnosed with scoliosis, this is based on two main characteristics: rotation and Cobb angle.
For scoliosis to be considered structural, the spine has to bend abnormally to the side, but it also has to coincide with rotation; this tells us it’s more than just a postural issue.
The spine’s abnormal curvature also has to measure at more than 10 degrees, and this brings us to what’s known as the ‘orthopedic gold standard’ for assessing scoliosis: Cobb angle.
If you are concerned that you, or a loved one, might have scoliosis, don’t be afraid to reach out; answers and treatment are only a click away.
Cobb Angle
As a progressive and incurable condition, it’s highly beneficial to spot the condition early on because this means treatment can also be started early on.
Cobb angle is one of the most commonly-used assessment methods for scoliosis.
A patient’s Cobb angle is obtained via X-ray images and tells us just how far out of alignment a patient’s spine bends and twists.
If we see that a patient’s spine not only bends abnormally to the side, but also rotates, the next step is to classify the condition on its severity scale; this helps guide our treatment approach moving forward and also indicates likely symptoms and rates of progression.
That being said, this only gives us an ‘idea’ of likely symptoms and progression rates as there are numerous factors that play into just how fast, or slow, a patient’s condition will progress.
A patient’s symptoms can also vary greatly across the board as there are multiple variables that go into determining how a patient experiences their condition: overall health-and-fitness level, condition form, age, location of the curvature, and condition severity.
Following are the Cobb angle measurements that determine condition severity:
- Mild scoliosis – cases where the Cobb angle measures at 25 degrees or less
- Moderate scoliosis – cases where the Cobb angle measures between 25 and 40 degrees
- Severe scoliosis – cases where the Cobb angle measures at 40+ degrees
Now that we have discussed Cobb angle and how it helps us classify the condition as mild, moderate, or severe, let’s move on to discussing some of the common symptoms of scoliosis.
What is Severe Scoliosis and What Does It Look Like?
We have discussed the stipulations that have to be met for a person’s scoliosis to be classified as ‘severe’, and we know that this must include a spine that bends abnormally to the side, rotates, and has a Cobb-angle measurement of more than 40 degrees.
This leads us to what I’m sure many of you are wondering: what does severe scoliosis look like?
To see what scoliosis actually looks like, you can refer to Mary’s X-ray image and see the abnormal bend to the side that characterizes the disorder.
Again, Mary is an example of a severe scoliosis patient who refused surgery and came to us seeking an alternative form of treatment.
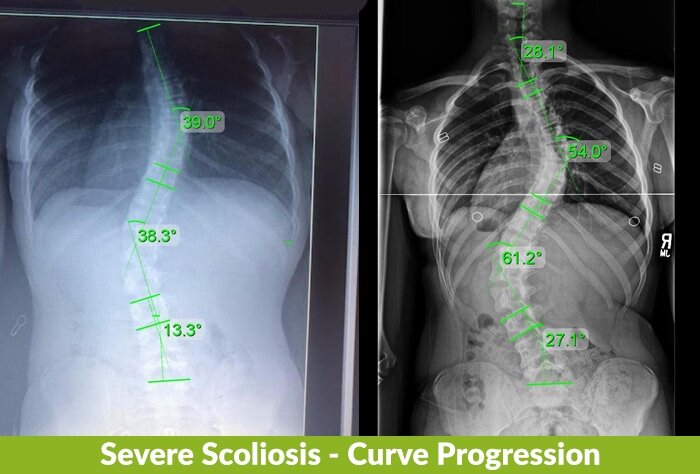
When I first saw Mary and her parents in 2019, they had decided to forgo active treatment. It wasn’t until they returned in 2020, after seeing Mary’s condition progress significantly, that they chose to commit to my treatment approach.
You can see, from looking at the images, how much progression can occur when left untreated.
Mary is a great example for showing that it’s never too late to seek out improvement through active treatment. While treatment might have been more successful if it had been started earlier, we were still able to impact the condition in a positive way.
While no two people with scoliosis will look and feel exactly the same way, let’s take a look at some of the common scoliosis symptoms that factor into just how visually noticeable a person’s condition is.
Common Scoliosis Symptoms
I always feel a little off using the term ‘common’ because when it comes to scoliosis, every patient is different, as are their symptoms.
That being said, there are some symptoms that are characteristic of the various scoliosis levels to watch out for.
Awareness of symptoms is important for parents and caregivers as early detection is as challenging as it is beneficial. There is a big connection between early detection and treatment success, assuming proactive treatment is started as close to the time of diagnosis as possible.
Severe Scoliosis
As each case of scoliosis is as unique as the person, the condition affects different people in different ways.
Add to that the fact that scoliosis develops across a wide severity spectrum, and you have a condition whose very nature necessitates a customized approach.

The farther along a patient gets on the progressive line of their condition, the more likely they are to significantly progress. In fact, cases of severe scoliosis carry a 90-percent risk of progression.
As a condition progresses, so does the likelihood of developing adverse symptoms and related complications.
It’s this high likelihood of progression that guides the recommendation, in the traditional treatment approach, for spinal-fusion surgery, and this is why every effort should be made early on to prevent reaching this stage.
Spinal fusion is invasive, costly, and comes with no guarantee that it will stop scoliosis from progressing. In addition, patients are often disappointed with their post-surgical pain levels, with some reporting an increase.
Once a person has reached the severe-scoliosis stage of progression, the symptoms mentioned for moderate scoliosis are even more pronounced and noticeable.
Let’s break the list of common severe scoliosis symptoms down and address each one individually.
Severe Scoliosis Pain
As mentioned earlier, mild and moderate forms of scoliosis are not known as painful in the condition’s most common form (AIS); however, around 20 percent of adolescents do report scoliosis-related muscle pain.
Adults, however, experience scoliosis-related pain very differently. As they have reached skeletal maturity, their spine is no longer lengthening, and as an abnormal curvature gets worse, there is no way to distribute that adverse spinal tension.
The spine then faces compression, along with its surrounding muscles, vessels, and nerves; this can negatively affect the body’s central nervous system and lead to persistent and chronic pain in the neck, back, arms, and/or legs.
Severe scoliosis hip pain is another common complaint as pain develops due to stretched ligaments caused by the misshapen spine.
The pelvis can also become tilted due to the abnormal curvature, and as one hip takes on more weight than the other, pain results from the misuse of the area’s muscles and tendons.
It’s important to remember, however, that focusing scoliosis treatment on addressing pain with pain medications or injections, instead of treating the whole condition, is not addressing the symptom’s underlying cause.
Here at the Center, we don’t focus our treatment on addressing symptoms, but on treating the underlying condition; that way, as a structural change is produced through active treatment, related symptoms like pain are lessened/eliminated throughout the process.
Postural Changes
The postural changes associated with severe scoliosis include more extreme forms of the changes common in moderate cases.
As an abnormal spinal curvature progresses, the body does its best to adjust. The larger a curvature gets, the more noticeable related postural changes can become.
Postural changes associated with severe scoliosis would include those mentioned for moderate scoliosis in a more extreme form, plus some additions:
- An overall asymmetry to the body
- Head appearing not centered over the body
- Shoulders that don’t sit at the same heights
- One shoulder blade protruding more than the other
- A more noticeable rib arch
- One hip that sits higher than the other, or appears more rounded/flat
- An uneven waistline
- Arms and legs that hang differently
- More noticeable changes to gait
- Balance issues
Sleep Problems
When discussing the symptoms of progressive and incurable conditions like scoliosis, the focus is often on the more extreme examples of physical changes, but scoliosis can cause a domino effect within the body that can produce a wide range of symptoms.
When a person is struggling with sleep due to an inability to get comfortable, back pain, or another scoliosis-related complication, this can greatly impact treatment efficacy, in addition to quality of life.
If a patient is not well-rested, it can be difficult to maintain a healthy mindset and keep up with the rigors of treatment.
If sleep problems are an issue for a patient, we will spend time discussing sleep habits, sleep position, and measuring them for a customized pillow that can help keep the spine in a neutral and aligned position during sleep.
Sleep problems can also be exacerbated by another potential severe scoliosis symptom: lung impairment.
Headaches
Living with scoliosis can produce a number of painful symptoms, especially in adult forms.
While headaches aren’t guaranteed to be a symptom of someone’s severe scoliosis, they are a common complaint.
Tension headaches can arise for patients with an abnormal curvature located in their cervical spine (upper back and neck); this can be caused by tight neck muscles placing tension on the head.
Scoliosis can also interfere with cerebrospinal fluid (CSF) flow, and this can result in a drop of CSF pressure in the brain.
These types of headaches, associated with scoliosis, can be debilitating and reach migraine levels.
Lung Impairment
Now, I should be clear, again, that the symptoms of severe scoliosis can range with some people experiencing them, and others not.
When it comes to lung impairment, for an average person living with scoliosis, even if there is lung impairment, it doesn’t commonly cause functional deficits, with many patients unaware as to how/if their lungs have been affected.
For professional athletes or people who place extra demands on their bodies and respiratory systems, this symptom can be more noticeable and cause some functional issues.
As is particularly the case with abnormal curvatures of the thoracic spine (middle-upper back), the curvature can push against the space used by the lungs to expand and contract. This can make it difficult to inhale/exhale deeply for prolonged periods of time.
As mentioned, lung impairment in severe cases can also impact a person’s ability to get a good night’s sleep as the natural breathing patterns during sleep can be disrupted.
Digestive Issues
It’s often the presence of scoliosis-related digestive issues that surprise people the most.
At first thought, what does the spine have to do with digestion? While the two might not seem overly connected, as the spine works with the brain to form the central nervous system (CNS), it can affect virtually every system at work within the body.
Scoliosis-related digestion issues can include difficulty with digestion and impairment of bowel function.
An abnormal curvature does have the potential to affect the digestive tract as much as it can affect the muscles closely surrounding the spine.

Living With Severe Scoliosis
We have talked about how a condition becomes severe and the characteristics that define this classification, but what is it actually like to live with severe scoliosis?
Again, every case is different, but generally speaking, severe scoliosis makes life more challenging for people and can affect them in a number of ways.
As severe scoliosis can cause persistent and daily pain, especially in adults, this can be disruptive to every-day life.
Pain can make it difficult to sleep, which can cause residual issues such as low energy and feelings of depression.
If a patient is experiencing a lot of pain, this can cause mobility issues, and in severe cases of scoliosis, spinal rigidity can also be a problem that can affect a person’s ability to engage in flexible movement.
As always, there is the psychological element of living with a severe form of a progressive condition marked by physical changes.
People with severe scoliosis tend to feel self-conscious about changes to posture, gait, and how their clothes fit; this can make them particularly sensitive to how they look and how people respond.
Patients at this level are the most likely to experience a heightened emotional reaction to the stress of their condition; this can come in the form of negative self-image, depression, or feelings of hopelessness for the future.
One of the most difficult aspects of reaching the severe stage of scoliosis is the pressure to make the right decision when it comes to treatment moving forward.
If you refer to the accompanying images of Kathy, you can see what the negative progressive line looks like structurally, not to mention how much the Cobb angle can change over four years.
As is the case with severe-scoliosis patients we see here at the Center, Kathy and her family decided to refuse the surgical treatment approach of undergoing spinal-fusion surgery.
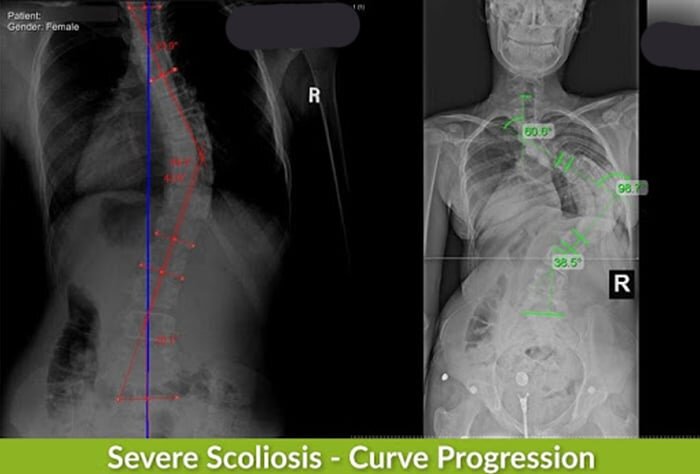
At this stage, for those on the traditional path of treatment, often spinal-fusion surgery is recommended; this procedure is costly, invasive, and comes with heavy side effects and risk of potential complications.
For those who feel surgery is their only option, this can increase feelings of powerlessness over their bodies, condition, and lives.
This is why I feel it’s so important that people know, even with severe scoliosis, there is another treatment option available.
I’m proud to be able to offer patients and their families a different way to treat severe scoliosis: a less-invasive option through a functional scoliosis-specific chiropractic approach.
Before we move on to the specifics of our approach for treating severe scoliosis here at the Center, let’s answer a question many people with severe scoliosis ask: is surgery really the best option?
Does Severe Scoliosis Require Surgery?
For years, when patients entered into the severe stage of scoliosis progression, spinal-fusion surgery was recommended as the best option.
For those following the traditional approach, they are funneled towards surgery as this approach does not include being proactive and working towards reducing the curvature early on in the condition’s progressive line.
Instead, patients undergoing traditional treatment are commonly told, when they are in the mild and moderate stage, to simply watch and wait.
Unfortunately, while everyone is watching and waiting, especially in AIS, when growth is still occuring, a rapid growth spurt can occur and speed up progression.
Instead of being proactive and addressing progression in a preventative manner, these patients are funneled towards surgery and might not be aware of other treatment options available to them.
While there is no doubt that treating severe scoliosis can be challenging, with commitment and hard work, there is a less-invasive treatment option available.
The issue I have with scoliosis surgery is that it’s costly, carries a lot of risks, is irreversible, and isn’t guaranteed to reduce pain, disfigurement, or permanently stop progression.
The ultimate goal of scoliosis surgery is to stop progression; it does this by fusing the most tilted-vertebrae of the curvature together so it heals into one solid bone, eliminating movement in that area of the spine.
Rods are then attached to the spine with screws to hold it in place while the spine continues to fuse and heal.
While this can work to stop progression, it does nothing to actually ‘correct’ the scoliosis, but rather holds the spine in a corrective position.
While this might sound successful in one regard, due to the fused section of the spine, many patients are disappointed with the lack of flexibility they are left with, and many also report an increase in back pain post surgery.
If a patient is unhappy with the results, the fusion fails, or there is a hardware malfunction, there is no recourse other than subsequent surgeries, and that is never a good thing.
Here at the Center, we treat our severe-scoliosis patients with an integrative and customized treatment plan that allows patients to avoid the potentially heavy and irreversible consequences of spinal-fusion surgery.
If you would like to discuss, in more detail, why surgery is not always the best treatment option, click here to contact us.
A Proactive and Functional Treatment Approach
Early in my career, I saw how patients with severe scoliosis were funneled towards spinal-fusion surgery, and I saw this as partially due to a lack of alternative scoliosis- treatment options.
Once there were other treatment options established, I saw that not enough people knew about them. This is why I wrote Scoliosis Hope, to educate and empower people by spreading awareness of other effective options.
I should also say that while my average severe-scoliosis patient is above the surgical threshold (between 40 and 60 degrees), most of these patients were told not to worry about their condition until it reached this surgical level.
In the severe-scoliosis cases we see here at the Center, prior to seeing us, these people have consulted with spinal surgeons and utterly refused to have the spinal fusion done.
Many of these cases continued to progress in the meantime, until they found us and our approach. With these patients, we take this into consideration when designing their treatment plan and do the best we can to alleviate any discomfort and bring improvement to their daily lives.
Here at the Center, every day I’m amazed to see the results that our severe-scoliosis patients can experience with some patience, hard work, and dedication.
If you refer to the accompanying images of Melanie, you can see the kind of positive improvement we are working towards with a curvature reduction.
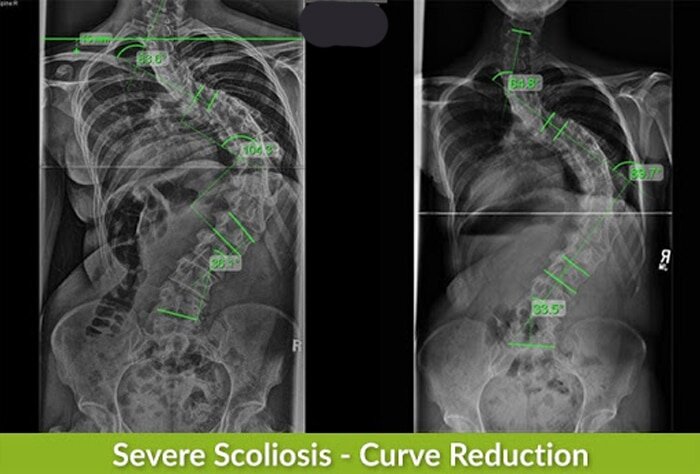
In Melanie’s case, she had reviewed all her treatment options and consulted with a surgeon about the option of spinal fusion.
Despite having the surgery recommended to her by the surgeon, she decided to refuse the invasive procedure, and by the time we met, she had progressed well beyond the surgical threshold.
Regardless, we implemented our alternative approach and were able to reduce her curvature, even though her case is still beyond the surgical threshold.
Had she come to me sooner, we likely would have seen even better results, but as things turned out, even though she still has a large curvature, our treatment reduced that curvature, along with related symptoms.
We work closely with our patients and engage them in the treatment process.
We use a combination of scoliosis-specific disciplines such as chiropractic, exercise, rehabilitation, and custom 3D bracing.
We apportion these disciplines accordingly so they complement each other and address each patient’s individual condition.
By working towards a curvature reduction, this addresses the structural nature of the condition and actually ‘corrects’ it, rather than merely ‘holding’ it in a corrective position, as scoliosis surgery does.
While it’s always better to try and avoid ever reaching the severe stage, it’s never too late to start treatment, and if the potential to avoid surgery is there, we jump on it.
If, for some reason, our approach doesn’t work, the patient can always return to the option of surgery, unlike the permanency of spinal fusion.
If you would like to know more about our proactive functional treatment approach, you can easily contact us by clicking here.
Bracing and Severe Scoliosis
Bracing is a component of scoliosis treatment that I would like to touch on.
The most commonly-used brace in the traditional approach is the Boston brace, but like surgery, the treatment goal of this brace is to stop progression, not to actually correct the abnormal curvature.
In some cases, squeezing braces like the Boston brace can cause more harm than good by actually weakening the spine.
Also, as Boston braces are uncomfortable, noticeable, and have to be worn virtually all the time, compliance can be an issue.
In our functional approach, as our goal is all about correction, we rely on a brace that has the potential to produce a corrective change: the ScoliBrace.
The ScoliBrace is fully customized to the patient’s body and condition, making it more comfortable to wear, and with correction as its goal, the ScoliBrace can complement other treatment disciplines by working towards a curvature reduction.
Now, there is still a range between severity levels within the severe-scoliosis category, and for some cases, especially in adults whose spines have stopped growing, bracing is not always an option, which is why surgery is often recommended.
In adolescents with severe scoliosis, bracing is more likely to be an option as their spines are still growing, and while bracing is more effective in the moderate stage, as are most facets of active treatment, the ScoliBrace can still impact cases of AIS with larger abnormal spinal curvatures.
Severe Scoliosis and Pain Management
When it comes to severe scoliosis pain management, there are better options than just taking pain-relief medication.
Those on the traditional treatment path are often prescribed pain medications or injections to address their scoliosis-related pain; this is because as there is a lack of active treatment while watching and waiting, not only is the curvature progressing unimpeded, pain is also not being addressed in a proactive way.
For those undergoing our proactive and functional treatment approach, we address pain by addressing the underlying cause of that pain; this is the difference between addressing a scoliosis symptom or the actual scoliosis.
Our therapy and rehabilitation includes exercises and stretches that not only augment our targeted chiropractic adjustments, but can also impact pain levels by keeping the spine and its surrounding muscles and tendons as loose as possible.
If pain management is addressed solely by medications, this can also be detrimental to treatment as pain can indicate progression, and if pain medications are masking that indicator, progression can go unnoticed, rather than being responded to proactively.
Frequently Asked Questions
What Degree Curve Is Considered Severe Scoliosis?
Scoliosis, a condition marked by an unhealthy sideways curvature of the spine, presents in varying degrees of severity, classified largely based on the Cobb angle measurement. A curve exceeding 40 degrees is classified as severe scoliosis, indicating a significant deviation from spinal alignment. This classification, crucial for determining the appropriate treatment approach, is part of a broader diagnostic process that considers key variables such as patient age, curvature location, and the condition’s cause. The progressive nature of scoliosis underscores the importance of early detection and proactive treatment to prevent worsening of the condition over time.
Severe scoliosis, particularly in adolescents, often results in noticeable postural deviations rather than pain, due to the ongoing growth that counteracts the compressive force of the curve. In adults, severe scoliosis can lead to increased rigidity of the spine, making treatment more complex and often necessitating a focus on pain management and spinal stabilization. Treatment approaches range from traditional methods, which may ultimately lead to spinal fusion surgery, to conservative, chiropractic-centered treatments aimed at correcting the curvature non-surgically. Early and proactive treatment can significantly improve the quality of life for individuals with scoliosis, reducing the likelihood of progression to a severe state and the need for invasive procedures.
What Makes the Treatment Approach at Scoliosis Reduction Center® Different for Severe Scoliosis?
The Scoliosis Reduction Center® takes a distinct, conservative approach to treating severe scoliosis, diverging from traditional methods that may lead to spinal fusion surgery. Their treatment philosophy is centered around a proactive, non-surgical intervention combining chiropractic care, physical therapy, corrective bracing, and custom rehabilitation exercises. This integrated approach aims not only to manage the condition’s progression but to actively reduce the curvature of the spine.
For individuals with severe scoliosis, this means a tailored treatment plan that addresses the structural deformity at its core, utilizing manual adjustments to achieve structural corrections, and then bolstering the spine’s support system through targeted exercises. This method is particularly effective for growing adolescents, where corrective bracing can augment the spine into a more natural position, and for adults, it focuses on stabilizing the spine and managing pain. The goal is to restore as much of the spine’s natural curvature, alignment, and functionality as possible, thereby improving the patient’s quality of life without resorting to invasive surgical procedures.
How Does Scoliosis Reduction Center® Address the Progressive Nature of Severe Scoliosis?
Understanding the progressive nature of scoliosis, particularly in its severe form, is fundamental to the treatment philosophy at the Scoliosis Reduction Center®. Recognizing that scoliosis is almost guaranteed to worsen over time without intervention, the center emphasizes early and proactive treatment to counteract the condition’s advancement. By initiating treatment soon after diagnosis, the center aims to not only halt but reverse the progression of scoliosis. This proactive stance is supported by a comprehensive treatment strategy that includes condition-specific chiropractic care, specialized physical therapy, and the use of corrective bracing tailored to each patient’s unique curvature and condition dynamics.
For adolescents, this approach is designed to leverage their growth phase to achieve maximum curvature reduction, whereas for adults, the focus shifts towards pain relief, spinal stabilization, and preventing further curvature progression. The center’s commitment to early intervention and its multifaceted treatment approach underscore its dedication to helping patients with severe scoliosis achieve the best possible outcomes, minimizing the need for invasive surgeries and enhancing overall quality of life.
Is It Too Late To Treat Scoliosis?
If you have severe scoliosis, is it too late for non surgical treatment? While surgeons may recommend surgery as the only relevant treatment option, I want patients and their families to know that alternatives exist.
When scoliosis becomes severe, treatment can be challenging for the patient — it requires a strong commitment, and results will not reveal themselves overnight. But I believe the difficulties faced by patients who choose less invasive treatment options pale in comparison to those who opt for surgery.
Numerous studies have highlighted poor outcomes for those who have been treated with surgery. And in many cases, a second surgery becomes necessary to remove hardware once the bone fusion has taken place. Surgery is not guaranteed to reduce pain, disfigurement or disability, either.
Here at the Scoliosis Reduction Center®, our patients with severe scoliosis amaze me with their hard work and commitment to improvement. Together, we treat the condition using custom plans designed for each individual patient. Through chiropractic care, exercise, rehabilitation and specialized bracing, patients can avoid surgery and make significant improvements in their ability to get the most out of life. And if, for some reason, the non surgical treatments do not work, patients can always choose surgery at a later date. I just want to make sure that patients and their families understand surgery is not their only option!
If you or your child are dealing with a case of severe scoliosis, you need to understand that not all roads lead to surgery! There are effective, alternative treatment options available. Yes, treatment will take time and effort, but it can help you find relief in a manner that is less invasive, less expensive and more personally empowering than surgery.
Conclusion
With varying degrees of severity, scoliosis can be classified as mild, moderate, or severe.
A patient’s Cobb angle is measured via X-ray, and this is how a condition is classified on its severity scale.
A designation of mild scoliosis is given to patients with Cobb angles of less than 25 degrees; moderate scoliosis for a Cobb angle measurement between 25 and 40 degrees, and severe scoliosis cases have Cobb angles of 40+ degrees.
Cases that reach severe status, whether they went undiagnosed until that stage or progressed to severe while watching and waiting, are more challenging to treat because they involve larger spinal curvatures.
While no two cases are the same, generally speaking, the larger the Cobb angle, the more likely it is that the patient will develop adverse symptoms and complications.
Common symptoms of severe scoliosis include a crooked spine that can be seen with the naked eye, postural changes such as an overall asymmetry to the body, pain (especially in adults), headaches, and potential complications such as lung impairment, digestion issues, trouble sleeping, irregular menstrual cycles, and difficulty maintaining balance and equilibrium.
Living with severe scoliosis can be difficult. In addition to the aforementioned symptoms, patients can also struggle with the emotional weight of having a severe progressive condition.
The more severe a progressive condition becomes, the more difficult it is to treat noninvasively; this is why, here at the Scoliosis Reduction Center®, our ultimate treatment goal is to reduce the size of the curvature so the patient never has to face the hardships associated with the severe stage of progression.
In terms of treatment options, there are two main approaches for patients to choose between: traditional and functional.
The traditional path is passive and involves watching and waiting until a condition is deemed severe enough to need spinal-fusion surgery, most often with curvatures over 45 degrees.
The functional path is proactive and involves initiating treatment as close to the time of diagnosis as possible; this is the approach we offer patients of the Scoliosis Reduction Center®.
Our approach is integrative and combines multiple scoliosis-specific treatment disciplines such as chiropractic, therapy, rehabilitation, and corrective 3D bracing.
As we take an integrative approach, we are better able to design fully-customized treatment plans that address the needs of the patient and the characteristics of their condition.
When it comes to addressing pain and other scoliosis-related symptoms, we do this by achieving a curvature reduction and impacting the condition on a structural level.
As we reduce an abnormal curvature and restore as many of the spine’s healthy curves as possible, we improve the spine’s overall biomechanics, which lessens/eliminates symptoms that were related to the abnormal curvature.
Consultation & Information Request
If you want to schedule a consultation, or just want more information you can call 321-939-2328 or use this form. We can call or email you to discuss your options.
